Have you ever been troubled with a yeast infection? Does your baby have a nasty diaper rash? It’s quite likely that you’ve experienced the effects of candida first hand at some point. Candida is a yeast (a kind of fungus) that is very common. It can be found practically everywhere – including our bodies. There are more than 20 species of candida that can cause infections. Our immune system usually keeps candida under control so that it doesn’t cause any problems. But an overgrowth of this fungi can mean trouble.1
Risk Factors
Some factors can make you more vulnerable to a candida infection.
- Sugar is a source of food for candida. So if you have diabetes and your blood sugar is high, you have a greater risk.
- If you have a weak immune system because of ill health, an autoimmune condition (like HIV or AIDS), medication, or chemotherapy, you’re more likely to develop an infection.
- Antibiotics can kill some of the “good bacteria” in our bodies. These bacteria are capable of stopping candida overgrowth. So if you’re taking antibiotics, you may be more vulnerable.2
Signs To Look Out For
Infection by candida is known as candidiasis. Symptoms can differ based on the part of the body that is affected.
Oral Candidiasis
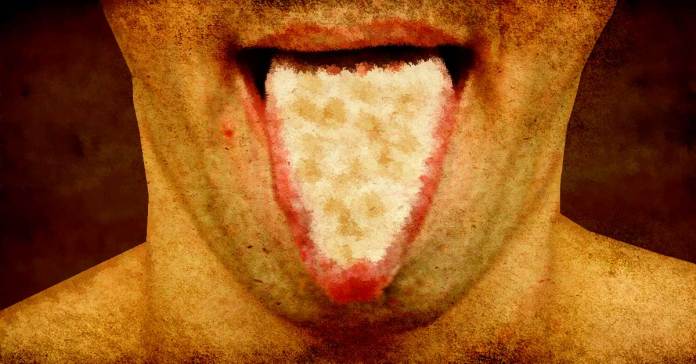
Oral candidiasis (thrush) is an infection of the mouth and tongue.3 Babies are commonly infected by candida in the mouth as their immune systems are not yet fully developed. As a result, an overgrowth of Candida albicans yeast in their mouth can lead to thrush. Sometimes, the mother and baby both get infected. In this case, you’ll need to be treated together to avoid passing the infection back and forth. You’re also more likely to develop thrush due to poor oral hygiene. Things like ill-fitting dentures can also trigger it.4
Several habits can help prevent an infection.
- Rinse your mouth out after you eat.
- Brush with a fluoride toothpaste twice a day and floss regularly.
- If you wear dentures remove them at night and make sure they’re clean.
- Stop smoking.
- Rinse your mouth with water after using a corticosteroid inhaler.
Symptoms include:
- White patches on the tongue or in the mouth.
- Bleeding when the white patches are wiped or scraped off.
- Bleeding during brushing.
- Trouble swallowing.
- An unappealing taste or loss of taste.
- Cracks in the corners of the mouth.
Babies with thrush may also become fussy or refuse to nurse. The mother may have cracked, sore nipples or pain while nursing if infected.5 6
Vaginal Candidiasis
Vaginal candidiasis (yeast infection) is a very common condition that affects most women. In addition to the other risk factors discussed, you’re more likely to get vaginal candidiasis if you’re pregnant.
Several habits can prevent an infection.
- Use plain water and mild, unscented soap to clean your genital area. Keep soap usage to a minimum, though.
- Avoid douching, which can eliminate healthy bacteria in the vagina. Don’t use greasy moisturizers or irritants like hygiene sprays or powders.
- Avoid wearing tight underwear made of materials like nylon. This can increase sweating, helping the fungus multiply.7
Symptoms of a yeast infection include:
- Unusual vaginal discharge ranging from a slightly watery and white fluid to a thick, white cottage cheese-like discharge.
- A burning sensation and itching in the labia and vagina.
- Pain when you have sexual intercourse or urinate.
- Reddish swollen skin around and in the vagina.
- White, dry spots on the wall of the vagina.
- Cracked skin in the genital area.8
Skin Infections
Candida can infect skin anywhere on the body. However, it’s most likely to grow in moist, warm parts with skin folds like the groin or armpits. It can also thrive inside a diaper and is the most common cause of diaper rash. Candida can infect the nails, too. Good personal hygiene habits and keeping skin dry can help prevent skin infections.
Symptoms include:
- A red rash in the folds of the skin, under the breasts, on the genitals, and other areas.
- Extremely itchy skin.
- Infection in the hair follicles that may look like pimples.
- Persistent diaper rash in babies.
- Abnormally shaped nails and infection of the surrounding skin.9
Invasive Candidiasis
In some cases, candida can enter your bloodstream and spread to various parts of the body like the heart, brain, bones, and eyes. This is a serious infection called invasive candidiasis.10 It is usually seen in those who have a severely compromised immune system due to conditions like HIV/AIDS, organ transplants, or chemotherapy. People who are taking broad spectrum antibiotics, have had recent surgery, or are diabetic are also at risk. Those on dialysis or are using a catheter may also develop invasive candidiasis.11
Depending on the part of the body that is affected, invasive candidiasis can cause a wide range of symptoms. Some initial symptoms may include a high fever (temperature of 38°C/101.4°F or higher), nausea, headache, and shivering. This should be treated as a medical emergency. In fact, if you’re at risk for invasive candidiasis, your doctor may recommend that you are admitted to the hospital as a precautionary measure.12
The Candida–Psoriasis Connection
Aside from causing candidiasis, the ubiquitous candida also contributes to psoriasis. This is a skin disorder characterized by flaky, reddish, crusty areas of skin, along with silvery scales.13 Candida has been found to exacerbate psoriasis.14 According to research, the quantity of candida in the saliva and feces of people with psoriasis is significantly higher than those who don’t have the condition.15
How Do You Treat It?
Antifungal medications (both oral and topical) are available to treat infections caused by candida. Candida is generally not contagious, though immunocompromised individuals may catch it.16
You can also try natural remedies. Yogurt contains extremely beneficial bacteria known as Lactobacillus acidophilus. This probiotic (good bacteria) can prevent the overgrowth of candida. One study found that eating 8 ounces of yogurt with Lactobacillus acidophilus daily was effective in reducing candidal infection.17 Garlic has also been found to inhibit the growth of candida. A sulfur-containing compound in garlic called allicin is thought to be responsible for this effect.18 Try chopping up some garlic for your salad dressing, sauce, or dip. You can also eat a garlic chutney.
References